WikkiTimes‘ Elijah Akoji uncovers how pregnant women deliver on cold floors under the care of traditional birth attendants in Kazurawa PHC, one of the neglected health facilities in Gaya Local Government Area (LGA) of Kano State, northern Nigeria.
Although Ibrahim Bala was the second child in a family of nine after his father and elder brother died in an accident, he knew that the bulk of the responsibility of caring for his aged mother and siblings after his father’s demise in 2019 rested on his shoulders. While he awaited his certificate from the Jigawa State Polytechnic, he started a phone business in Gaya and catered for his family with the little he made.
“The hope was that after the result comes out, he will get a better job and give the family a good life; he was our light,” Danjuma, a younger brother to Ibrahim said outside their family home in Kazurawa.
Ibrahim died in the heat of the cholera outbreak that claimed hundreds of lives in Kano state in 2021.
One evening in August, while he was out meeting with friends, he began to complain about his stomach, saying he needed to go home. Ibrahim’s younger brother and some friends accompanied him and, upon getting to his house, he started stooling.

“No one knew what the problem was, and we did not know what to do. We prayed that he would get better, but it got worse. He started vomiting too,” Danjuma told WikkiTimes.
Unknown to the family, it was cholera. All they knew was that he needed medical attention, and he was rushed to Kazurawa Primary Health Care Centre.
The health facility was in a deplorable state, with the only member of staff, a nurse, doubling as the midwife and pharmacist.
“The only treatment he got was the drip he was placed on for some hours. If he had gotten the best attention and drugs, my brother wouldn’t have died,” Danjuma added.
HEIGHTENED MATERNAL MORTALITY
Ibrahim’s family wasn’t alone in their suffering. For Aisha Suleiman, September 12, 2021, was a date she would never forget. She was rushed to the health centre after her contractions started at about 1 am. It was still in the peak of the rainy season and parts of the roof had pulled off, exposing the entire health facility to rain.
Aisha was admitted into a room with no windows or doors and part of the roof pulled off. In her vulnerable state, she was forced to wait in an exposed ward for the traditional birth attendant (TBA) who stayed some kilometres away from the health facility. Long before the arrival of the TBA, Aisha began to bleed.
“I will never wish anyone, even my enemy, to go through my experience. I was in pain with no help. I was exposed to cold because it was still raining when I was rushed to the hospital. It was when the traditional birth attendants came that they discovered my baby had already died because my water had broken for so long and the baby couldn’t survive anymore. I totally lacked the care every pregnant woman deserved,” Aisha said.
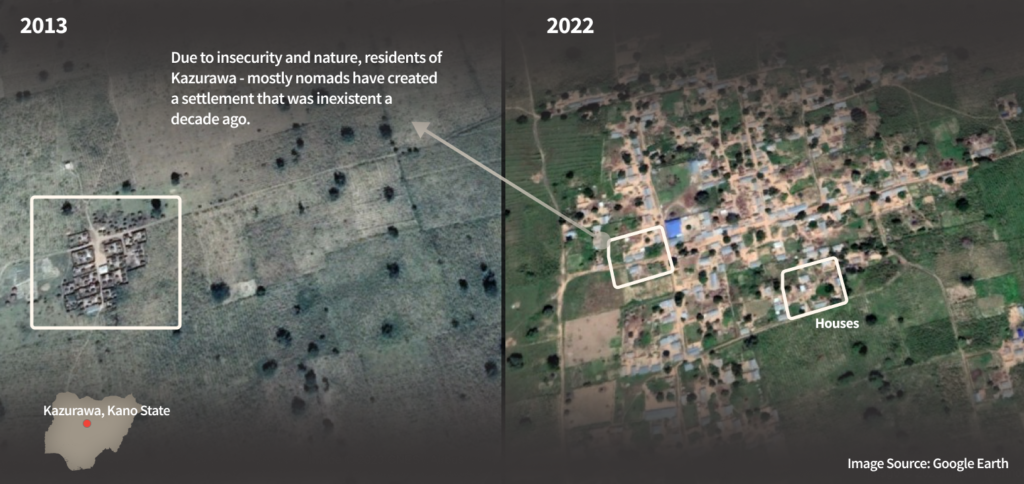
Nigeria accounts for almost 20 per cent of global maternal deaths. The prevalence of maternal mortality in Nigeria is very much connected to the state of primary healthcare centres in the country and inequities in access to health services. Primary healthcare is the first level of contact of individuals, families, and communities in providing services to the majority of people based on need without geographical, social or financial barriers.
Maryam Jibril, who gave birth three months ago at the healthcare centre, recounted how her three years old daughter was admitted to the health facility on a mat because there was no functional bed available. But this unfortunate experience didn’t surprise her.
“As a pregnant woman, I was kept on the same mat for two days before they made a provision and admitted me. The whole health facility looks empty and in bad condition,” Maryam said.
Idris Muhammed, the officer-in-charge of Kazurawa Primary Health Centre, said the health facility had been abandoned.
“For the past two years, the condition of the health facility is getting worse. Now, we can’t take deliveries. If we must, then we must call the traditional birth attendant. There is no ward to admit sick patients, no drugs, and no staff; I am the only staff here at the health facility (oic),” Idris said.
KANO CHOLERA OUTBREAK
Ibrahim was one out of the 369 deaths recorded in Kano state during the cholera outbreak in 2021. Between March 2021, when the outbreak started, and June 22 of the same year, 119 deaths were recorded in a caseload of 3,209 across 33 of the 44 local government areas in the state. Gaya and Bichi LGAs had the highest number of infected persons.
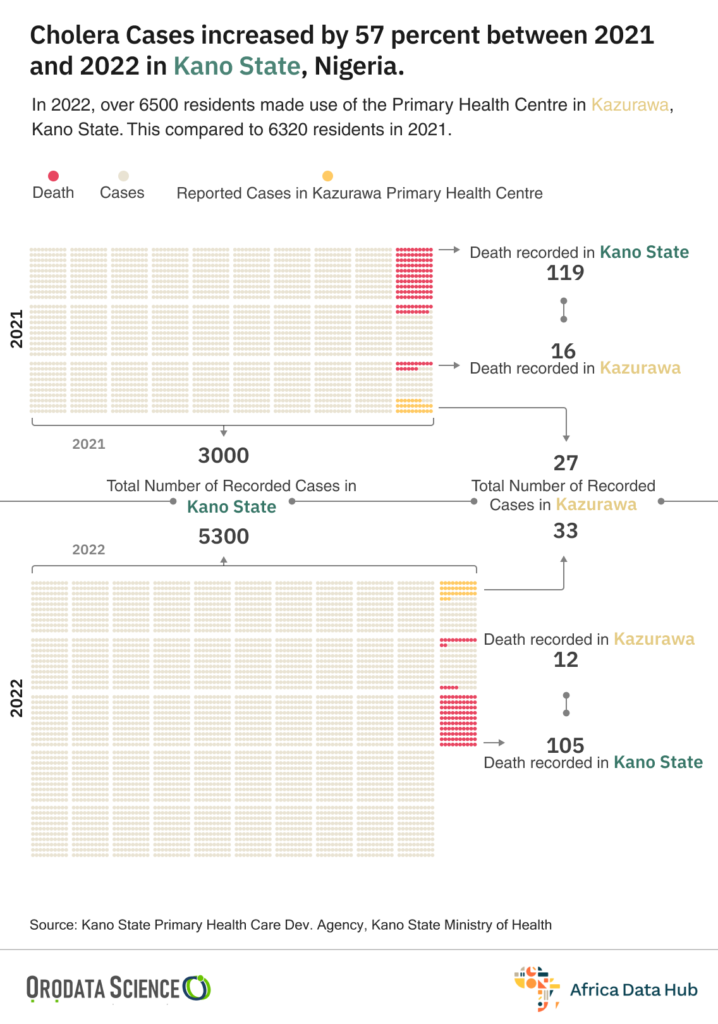
A cursory look at the cholera figures showed the government’s poor epidemic preparedness and management. In July 2021, the number of cholera casualties rose from 119 to 169 out of 5221 cases in the 41 LGAs hit by the outbreak. In August, the figure rose further to 173 out of 5316 laboratory-confirmed cases.
A month later, 329 people died with the number of laboratory-confirmed cases rising to 11,475 across the entire 44 LGAs in the state. Gaya LGA ranked the highest with over 2,000 cases.
FINANCIAL MISAPPROPRIATION

The Primary Healthcare Centre in Kazurawa community in Kano State is in deplorable condition despite the N3 billion provided by the state Primary Health Care Management Board in 2021 to fix healthcare centres in the state.
The decrepitude of the healthcare centre that was serving thousands of Kazurawa dwellers contributed to the pain and anguish residents felt. Many pregnant women lost their babies while sick patients risked their lives to the inadequate treatment provided by the only health facility available to the residents of the community.
WikkiTimes reported that in the same year, the Kano Ministry of Health received N30.720 billion to address health issues in the state.
READ: Recruited to Suffer: Over 12 months Unpaid Salary, Arrears, Frustrate NBAIS Workers
In its Q1 2021 budget performance report, the state reported it had spent N2.899 billion on healthcare. Its Primary Health Care Management Board also approved a N3.021 billion budget for the rehabilitation and maintenance of primary healthcare facilities in the state.
Despite the billions of naira earmarked for improvement of healthcare delivery in the state, and the state government’s reported “great work” in primary healthcare delivery, the only healthcare facility in Kazurawa remained neglected.
The Kano state government should work to reduce the mortality rate of its citizens by improving medical equipment and facilities and supporting communities to implement affordable and effective access to medical services.
This report is done with support from the African Data Hub.