In recent times, Benue state has been confronted with the outbreak of different diseases leading to the death of many residents. To address this challenge, the state government prioritised the health sector in its yearly budget but this has not translated to the desired impact at the primary healthcare level. In this report, Ekemini Simon, showed that lack of political will by the state government, and not financial resources, is the bane of healthcare development in the state.
Yusuf Ibrahim, 16, from Obagaji, Agatu in Benue State, had great prospects while growing up. In academics, he was always top of his class. At home, Ibrahim was also very helpful in cultivating several farmlands that supported the family. Yet, Ibrahim had something unique that made him renowned in his neighbourhood. He was famous for volunteering to repair faulty electronics and bicycles in his community, and he recorded several successes with little pennies as income and attracted public admiration to the extent that he was widely referred to as an engineer by his admirers.
“He was our shining star and we were ready to support him to pursue his Engineering dreams to the University upon graduation from secondary school,” said Haruna, Ibrahim’s uncle, at his home in Obagaji, Agatu Local Government Area (LGA), Benue State.

Unfortunately, those dreams never materialised, as Ibrahim died in the heat of the cholera outbreak that claimed 14 lives in his community in January 2021. Haruna said Ibrahim’s plight started with stomach pain after he had taken dinner. They thought it was a mere stomach pain but were alarmed when he started vomiting and started passing watery stool.

“When that happened, we rushed to a local pharmacy for drugs. The drugs did not address the problem and he later died,” Haruna said.
Asked why Ibrahim was not rushed to the Primary Healthcare Centre (PHC) in the community, Haruna said, “Everything happened so fast. But the thought of going to the PHC is far off. The place is not functional at all. Sick people rarely visit the place. You won’t even find drugs, not to mention medical equipment. So, we were often left with the choice of getting drugs from chemists.”

The story is not different from a nearby local government area, Guma. In Kabawa community in Abinsi, Guma LGA, many residents recount how their kindred lost their lives trying to access the only functional PHC in the local government area at Gbajimba which is 16 kilometres from their community.
READ: How SUBEB Awarded Contracts To Inactive Contractors, Non-existent Schools In Kano
“It is only the Primary Healthcare Centre at Gbajimba, which is the Governor’s community that was manageable then. So, when we had cholera outbreak, we rushed people there but some died on the road because of the long distance. Everything happened so fast and delay in medical attention cost lives,” said Iliya Ali, a resident of Kabawa community.

Ali told Solacebase that if Kabawa community had a functional PHC, his bosom friends, Umar Abubakar and Kawu Ibrahim, who were victims of cholera outbreak would still be alive.
The Kindred Head of Mbanyiar, Mbawa council ward, Guma LGA, Zaki Pius Wergba added that during the cholera outbreak, the PHC in his domain, Daudu, lacked the basic facilities to attend to patients and that those affected were rather referred to the General and Teaching Hospitals in the state capital, Makurdi.
Authorities in Guma LGA told Solacebase the PHC at Tse-Iordye, which was upgraded through the intervention of Victim Support Fund (VSF) and Red Cross has remained non-functional due to frequent attacks from herdsmen who have now taken over the community and forced residents to desert the area.
Cholera, a water-borne disease characterised by sudden onset of profuse watery diarrhoea, is known to lead to premature death as a result of dehydration, if not managed on time. Other symptoms of cholera include nausea, vomiting, and weakness.
In 2014, no fewer than 35 persons were reported dead, in addition to over 200 persons that were infected by cholera. Six years earlier, that same number died from the outbreak.
In January 2021, 26 people were reported dead with over a 100 cases of infection in Agatu and Guma LGAs. The outbreak was linked to contaminated water sources according to residents and reports.
Primary healthcare takes a back seat in Benue
A cursory look at the recent history of the cholera outbreaks in the state reveals a disturbing trend of lack of priority and poor epidemic preparedness by the state government. According to the official website of the state’s ministry of health, its primary goal is to maintain the health security of Benue citizens, however, the reality on ground suggests otherwise.
Findings by Solacebase revealed that one of the underlying reasons for repeated deaths from cholera epidemics in Benue state, is due to the widespread dearth of its primary healthcare system. For instance, during the cholera outbreak in January 2021, most PHCs in the state particularly those in Guma and Agatu local government areas lacked medical supplies such as drugs, intravenous (IV) fluids among other essential facilities, in addition to deficient staff-to-patient ratio, and poor infrastructure to accommodate patients.
According to medical officers and community leaders in Guma and Agatu local government areas, the key support they have received over the years for their PHCs come from interventions by donor organisations such as the International Community of the Red Cross (ICRC), Victims Support Fund, Federal Government Basic Healthcare Fund and Disease Surveillance and Notification Officers (DSNO).
Immunisation Officer, Guma LGA, Dr. Adega Aondoade recounts that when cholera struck last year, there were neither vaccine nor test kits in all the PHCs in the local government. He added that the Red Cross intervened by supplying IV fluids at the General Hospital, Gbajimba, and that proved very useful especially amongst children who were presented for early treatment.
Aondoade said that even Gbajimba PHC which happens to be where the Governor, Samuel Ortom, hails from is the only PHC relatively modest to cater for patients in the entire local government area. Gbajimba PHC attained its current status through the intervention of Victim Support Fund (VSF) and Red Cross, who rebuilt it when militia herdsmen burnt it down including people’s houses in 2014.
The immunization officer noted that the advantage Gbajimba PHC has is its affiliation to the Benue State University Teaching Hospital (BSUTH), Makurdi where they refer cases that are beyond their control.
The officer-in-charge (OIC), Gbajimba PHC, Eunice Chindo, explained that the Red Cross built a perimeter fence, and toilets while VSF built a structure for maternity ward. Commendably, the state Primary Healthcare Board took the responsibility to build staff quarters and also provided electricity.

However, this was not enough during the outbreak. Chindo said at the onset of the cholera outbreak, the facility lacked drugs and important medical equipment.

”We have enough equipment now to tackle Cholera because during the outbreak the state government started making supplies. Measles came and we were able to tackle it.”
Not many PHCs received this type of interventions across the state. According to the officer-in-charge of Daudu PHC, Felicia Amaka, the major problems bedevilling the facility includes unavailability of buildings that could serve as wards and staff quarters, lack of equipment and drugs.

She said: “There was a time we had an outbreak of measles but there was no space. During the outbreak of cholera, people did not even care to come to us. Even when Covid-19 came, we still did not have space.
READ: FG Fails To Deliver 90km Panyam-Bokkos-Wamba Road 15 Years After, Despite Billions In Releases
“We only have space for six beds which is not enough for the population we have here. We only have two wards and this is not good for a maternity unit. We also have a serious challenge of shortage of staff and it is not only in this centre but the situation is the same across Guma LGA.

“We have few staff on the payroll, the rest are volunteers who can quit at any time. If the government can engage them as real staff, it will help us a lot. If there is another Cholera outbreak, we will not be able to tackle it because we are lacking necessary equipment.”
In Agatu LGA, the Director of Health, at the LGA headquarters, Anna Adebo, told Solacebase that out of 54 PHCs across Agatu, less than 20 percent is operational and are in a deplorable state.
“Presently, most of the facilities that are working lack the capacity to provide essential health-care services. In addition to having issues such as poor staffing, inadequate equipment, poor distribution of health workers, poor quality of health-care services, poor condition of infrastructure, and lack of essential drug supply.

“The dilapidated structures need to be reconstructed to meet modern standards. We have about 54 PHCs across Agatu but sadly they are not in good condition. So we call on the federal, state and local governments to give maximum attention to them so that it will serve the people of Agatu better. However, the state government has been trying, but they need to do more.”
The traditional ruler, Agatu, HRH, James Ochadoji corroborates this position.
“It will interest you to know that most PHC facilities here in Agatu are in various states of disrepair, with equipment and infrastructure being either absent or obsolete, the referral system is almost non-existent. Who knows? Perhaps if the facilities were working, we wouldn’t have recorded such a number of deaths during the Cholera outbreak,” he said.
It is noteworthy that majority of the PHCs visited across rural communities in Guma and Agatu local governments don’t measure up to the minimum standards of PHCs jointly set by the Federal Government and World Health Organisation (WHO). According to the standards, a PHC should have a detached building with at least 13 rooms whose walls and roof must be in good condition with functional doors and netted windows, functional separate male and female toilet facilities with water supply within the premises, and availability of a clean water source; at least motorized borehole.
Others facilities should include sanitary waste collection point and waste disposal site, connection of the facility to the national grid and other regular alternative power sources, signpost- visible from both entry and exit points, fenced with gate and generator houses, staff accommodation provided within the premises, and pharmacy and dispensing unit.
The minimum standard also stipulates that medical equipment such as clinical thermometers, cord clamps, Cusco’s speculum, dressing forceps, dressing trolley, enema kits, episiotomy scissors, foetal stethoscope, kidney and dishes. For non-medical equipment, there must be availability of delivery bed, examination couch, observation beds, wash hand basin, wheelchair, and writing table.
Furthermore, the standard stressed that a PHC should have 19 medical personnel and 5 non-medical personnel. This medical personnel include nurses, pharmacy technicians, health assistants, laboratory technicians and medical records officers.
Government poor spending priority behind avoidable deaths and suffering in Benue
The poor condition of medical facilities across communities in Benue state is not a happenstance. It is reflective of the state government’s poor spending priority on primary healthcare and how much it values the health of its citizens.
Interestingly, analysis of the appropriation laws of Benue State gives credence to the fact that the state government recognises the poor state of its medical facilities but lack the political will to confront the issue.
Solacebase checks into the Benue State budget in 2020, a year of covid-19 outbreak, and a year before the Cholera outbreak, show that there were budgetary provisions by the state government to address the need for medical equipment, essential drugs and medical facilities.
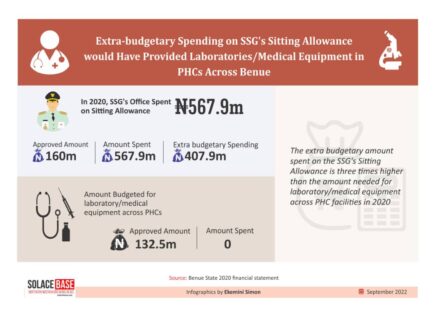
For example, in the 2020 budget of Benue State Primary Health Care Board (BSPHCB), the state budgeted N596.2 million for the implementation of capital projects across PHCs in the state. Interestingly, N132.5m out of the N596.2m was earmarked for the provision of laboratory and medical equipment in the state.
Yet, checks into the 2020 Benue State financial statements showed that no funds were released for the provision of laboratory and medical equipment nor a dime for any project across PHCs in the state.
Extra budgetary spending in the governor’s office, SSG would have prevented avoidable deaths
Findings showed that paucity of funds was not the challenge to the Benue State Government in addressing the dearth of infrastructure in PHCs across the state. In 2020, a year the government needed to prioritize spending on healthcare due to covid-19 outbreak among other infectious diseases, there were questionable expenditure by the state government, which could have been redirected to fund efficient and quality service delivery across PHCs in the state, thus saving lives.

For instance, although the office of the Secretary to the State Government had approval to spend N160 million for Honorarium and Sitting Allowance in his office, the office went beyond the approval to spend N567.9 million. The extra expenditure of N407.9 million is three times higher than the amount needed for the medical equipment across the state PHCs in the same fiscal year.
What is more, the extra budgetary spending perpetuated through the welfare package of the governor, amounting to N177.1 million, when added to that of the SSG (N407.9 million) could cater for at least over 98 percent of the total N596.2 million budgeted for capital expenditure by the BSPHCDA in the year 2020.
“Our Attention more on Secondary, Tertiary Healthcare” –health commissioner
Benue State health commissioner, Mr. Joseph Ngbea told Solacebase that the Governor Ortom-led administration prefers to give more attention to secondary and tertiary health care than primary healthcare.
He claimed, the reason for this choice is because people do not believe much in primary healthcare services.
“People do not believe in primary healthcare. However, awareness is still created. Because of this, we give more attention to tertiary and secondary healthcare. That is the reason, if you go to the Teaching and General Hospitals, you will see the medical equipment we have provided,” he said.
Ngbea said he cannot comment specifically on why attention was not given to medical facilities in Guma and Agatu LGAs before the cholera outbreak since he was not the Commissioner for Health prior to the outbreak.
He said “What I can say is that the Government cannot renovate all of them (PHCs) at the same time. I was not the Commissioner for Health that time. I was appointed on December 21, 2020 but resumed duty in January 2021. My first duty as a Commissioner was to contain the cholera outbreak. I drove there myself with the permanent secretary with consignments to go and give them.”
The commissioner, however, noted that work has commenced on the renovation of three PHCs in the State. They are Agasha Comprehensive Healthcare Centre, Nzorov PHC in Guma LGA and Gyura PHC in Gboko LGA.
He added that: “In the next two weeks, the Governor will provide some funds through the Central Bank to the ministry. I can assure you that it will be used more to develop Primary Healthcare. When that is done, I will beat my chest and say that I have tried. When the next commissioner comes, he will take it from there.”
Government must give more Attention to Primary Healthcare – PPDC
A non-governmental Organisation, Public and Private Development Centre (PPDC) has said that it is important for the government to prioritize funding for the primary healthcare centres.
Reacting to findings in this report, the Programs Manager, PPDC, Nonye Akubuo, in an interview with Solacebase said the need to prioritise funding for the PHC is because it is healthcare for the grassroots.
“You cannot say you give more attention to secondary and tertiary health and then abandon or give less premium to primary healthcare services. If you ignore the foundation, then what you do at other stages would be faulty,” Akubo noted.
Akubo said the reason many may have preferred secondary and tertiary health care service is primarily because of the noticeable gaps in PHCs.
“In many PHCs, you hardly find medical personnel because of the inconveniences of facilities. You rarely find drugs among other medical equipment. This discourages people from going there.
” If the government becomes intentional in giving adequate attention to PHCs by providing the standard facilities recommended by the National Primary Healthcare Development Agency including preference to staff welfare, it will boost confidence in this very important healthcare service and then people will start using it and more lives will be saved.”
This republished report is produced with support from the Wole Soyinka Centre for Investigative Journalism (WSCIJ) under the collaborative Media Engagement for Development, Inclusion and Accountability project (CMEDIA) funded by the MacArthur Foundation.